The common fatty liver causes are:
- Sugar
- Simple carbohydrates
- Our body fat, when in excess

The Name Fatty Liver can be Misleading.
The name Fatty Liver can be misleading us to think that it is the fat we eat causing the problem. Fat is usually blamed for and focused on because of:
- its name and
- the fact that eating it can spur on very uncomfortable symptoms when the liver is fatty.
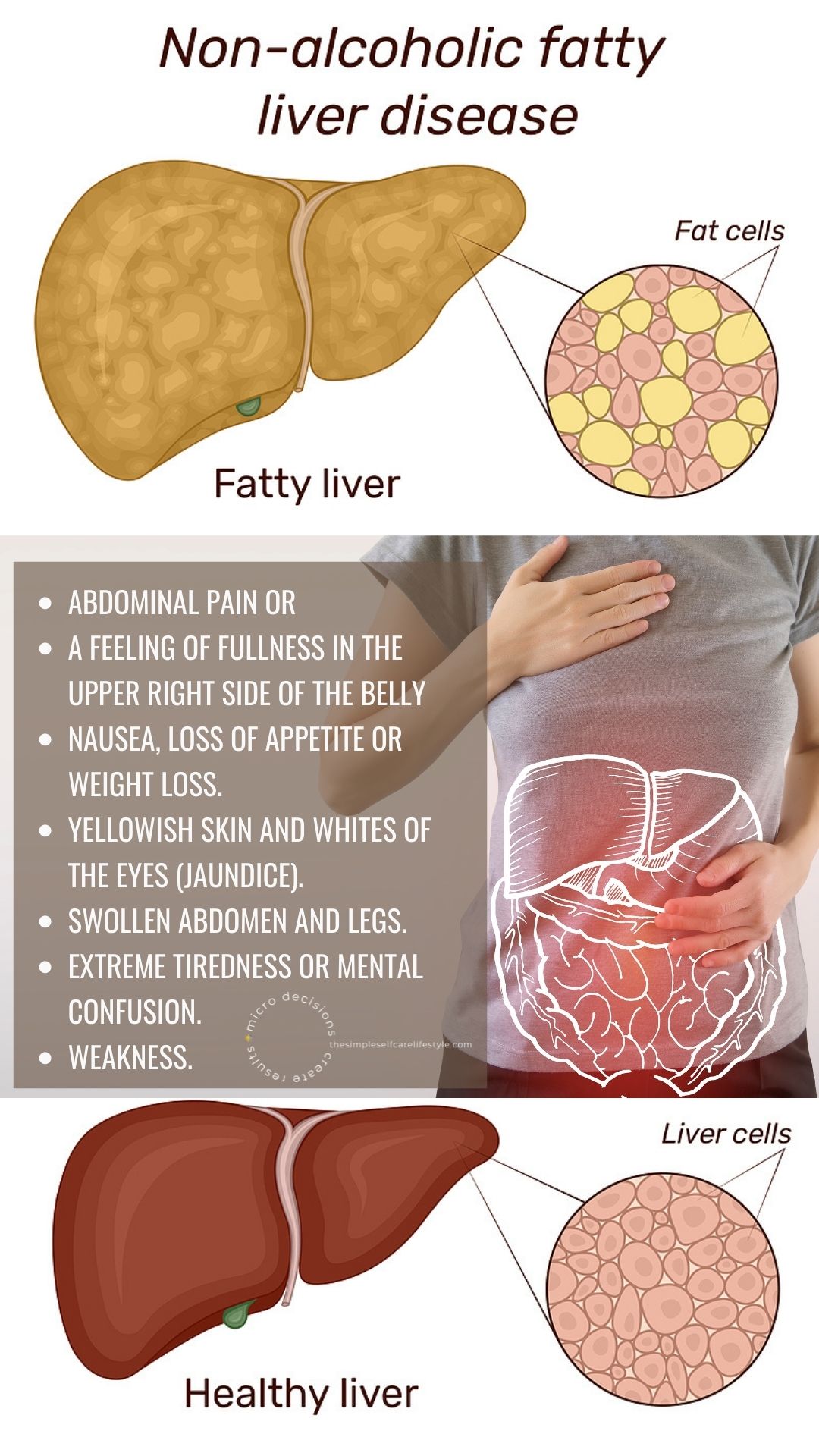
Eating Fat Can Cause Symptoms so Eating Lean While Healing A Fatty Liver May Be Necessary.
Uncomfortable symptoms arise when the liver is struggling with too much-stored fat.
It is the Fatty Liver that makes it harder for the fat we eat to be handled by the Liver.
This means even the ‘good fat’ we eat may need to be reduced for a while as we heal the Fatty Liver.
Bad fats should always be eliminated anyway. But it is important to know it is NOT the fat causing the Fatty Liver. The Fat provokes a SYMPTOM of a Fatty Liver.
We must reduce the CAUSE to help the Liver heal.
Discomfort After Eating Fat is a Symptom
Discomfort after eating fat is a symptom of the fatty liver condition and, according to Dr. W. Daniel Jackson, is not the cause.
That is very important to know because if the focus is only on reducing fats to avoid discomfort, the root causes will never be addressed.
Sugar – Simple Carbohydrates – Excess Body fat
Sugar – simple carbohydrates – excess body fat are where to place focused actions when it comes to helping fatty livers get better.
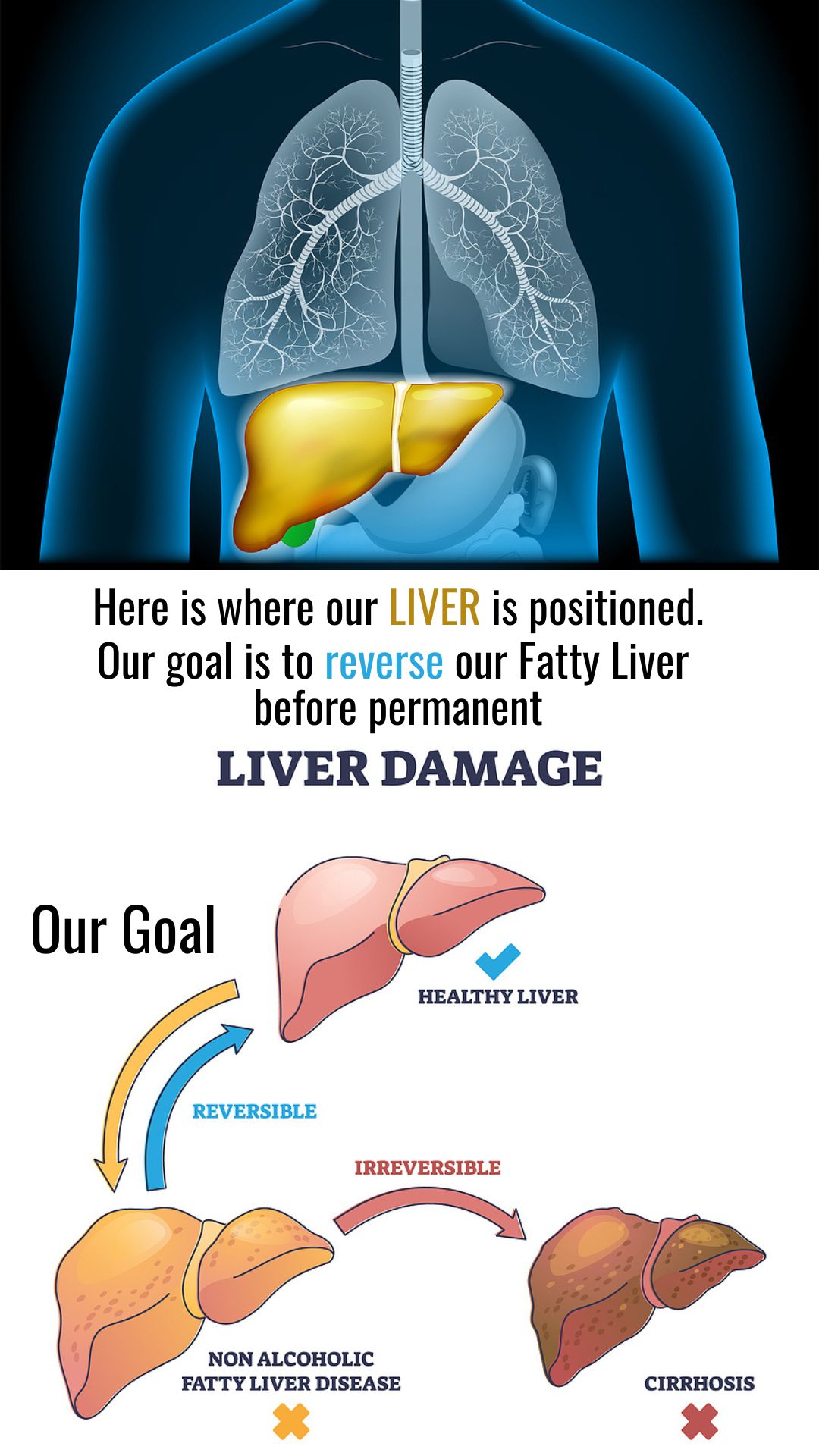
How Does a Liver Become Fatty?
To unwind a fatty liver and lighten its load, we need to know what is making it fatty.
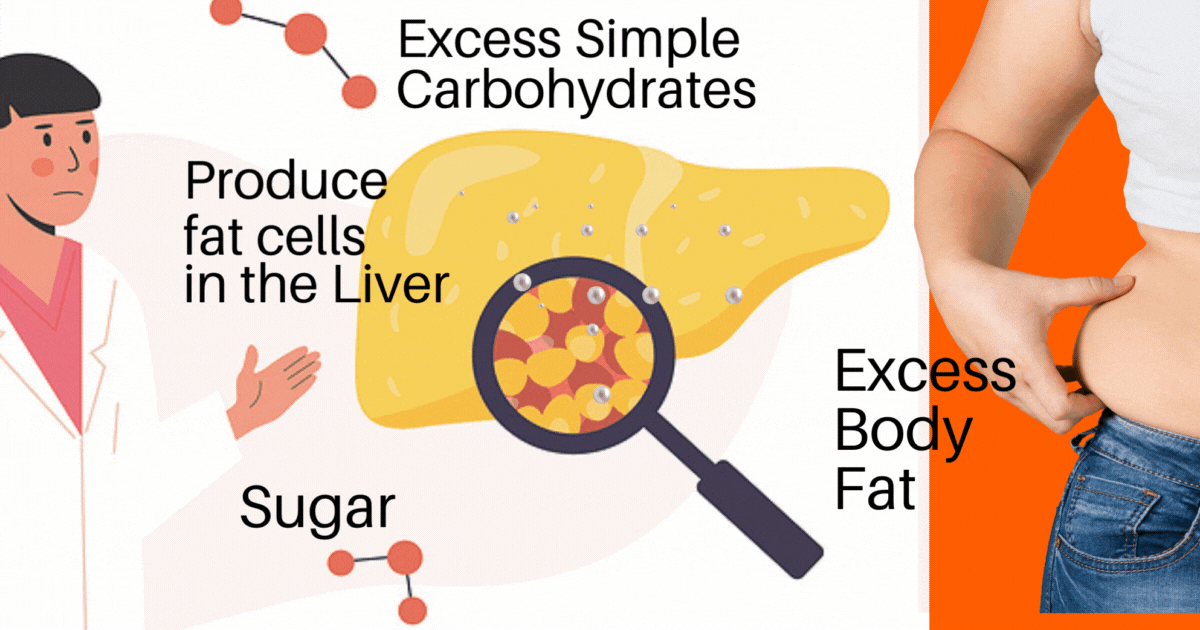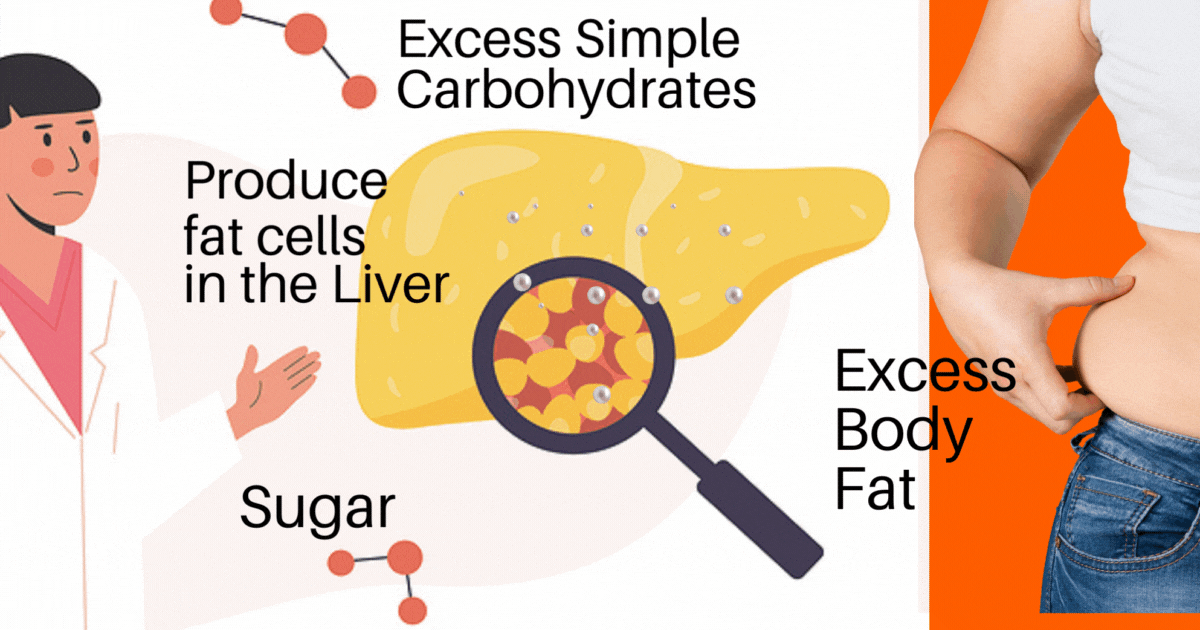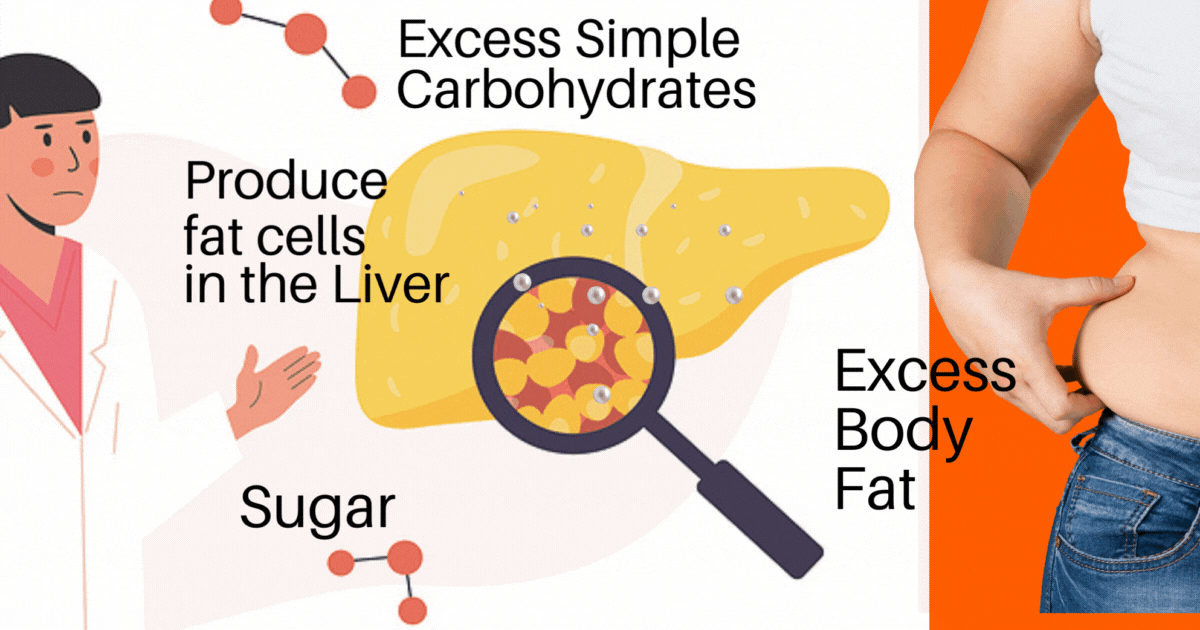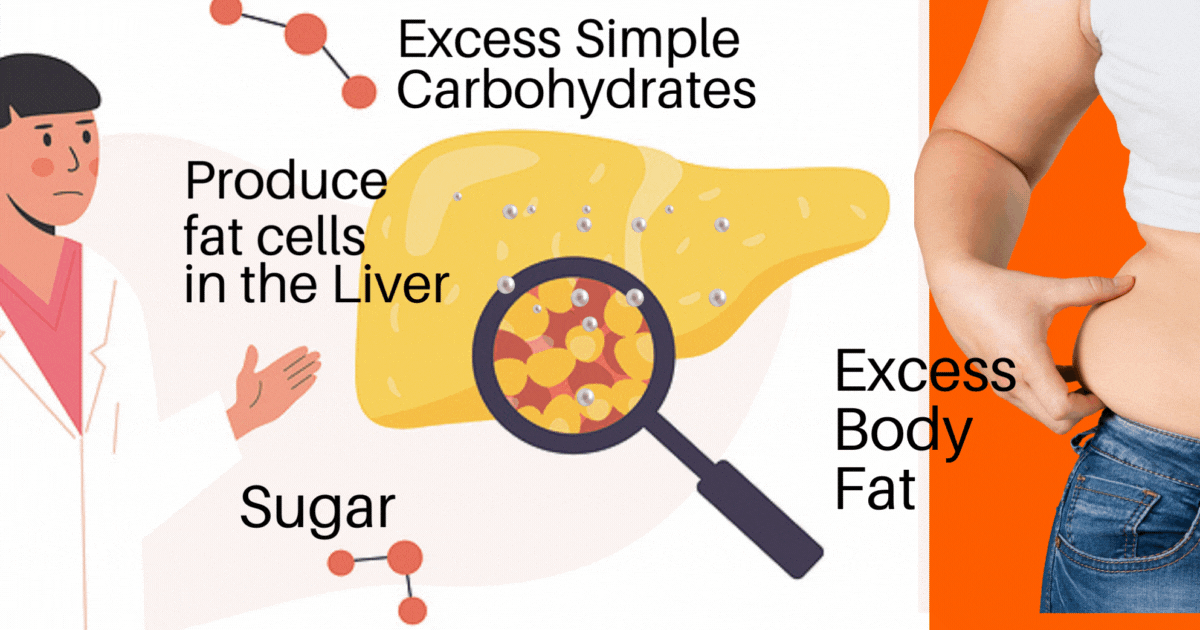
An oversimplification of the process of how a fatty liver develops is:
1. Sugar in excess (glucose, fructose, and the 2 together = sucrose [table sugar]) is converted to (triglyceride) fat and
2. Simple carbohydrates in excess are also converted to (triglyceride) fat. Simple Carbohydrates (think bread, bagels, pasta, crackers, cookies, processed foods, and things made of flour).
The excess (triglyceride) fats get stored in the liver and start adding up until there is just too much.
It all started with too much Sugar and Simple Carbohydrate. The excess is converted to a fat called triglyceride, and that ‘triglyceride’ fat is clogging up the Liver.
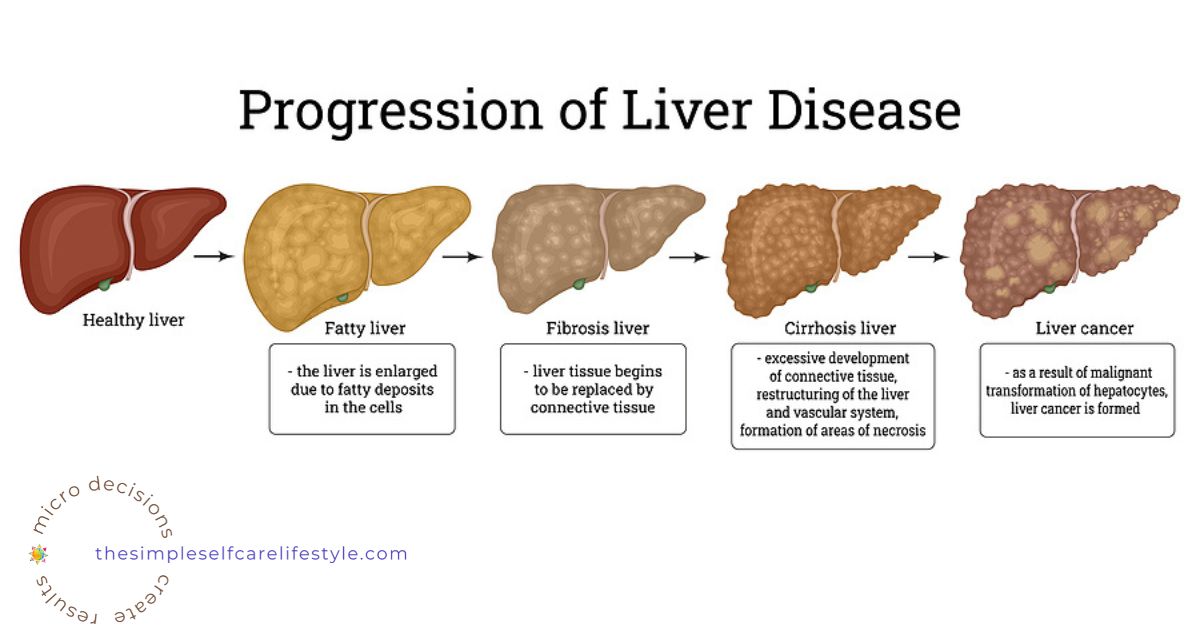
As this scenario continues, the liver cells start to be overtaken by fat cells. The liver gets too stuffed, and it enlarges.
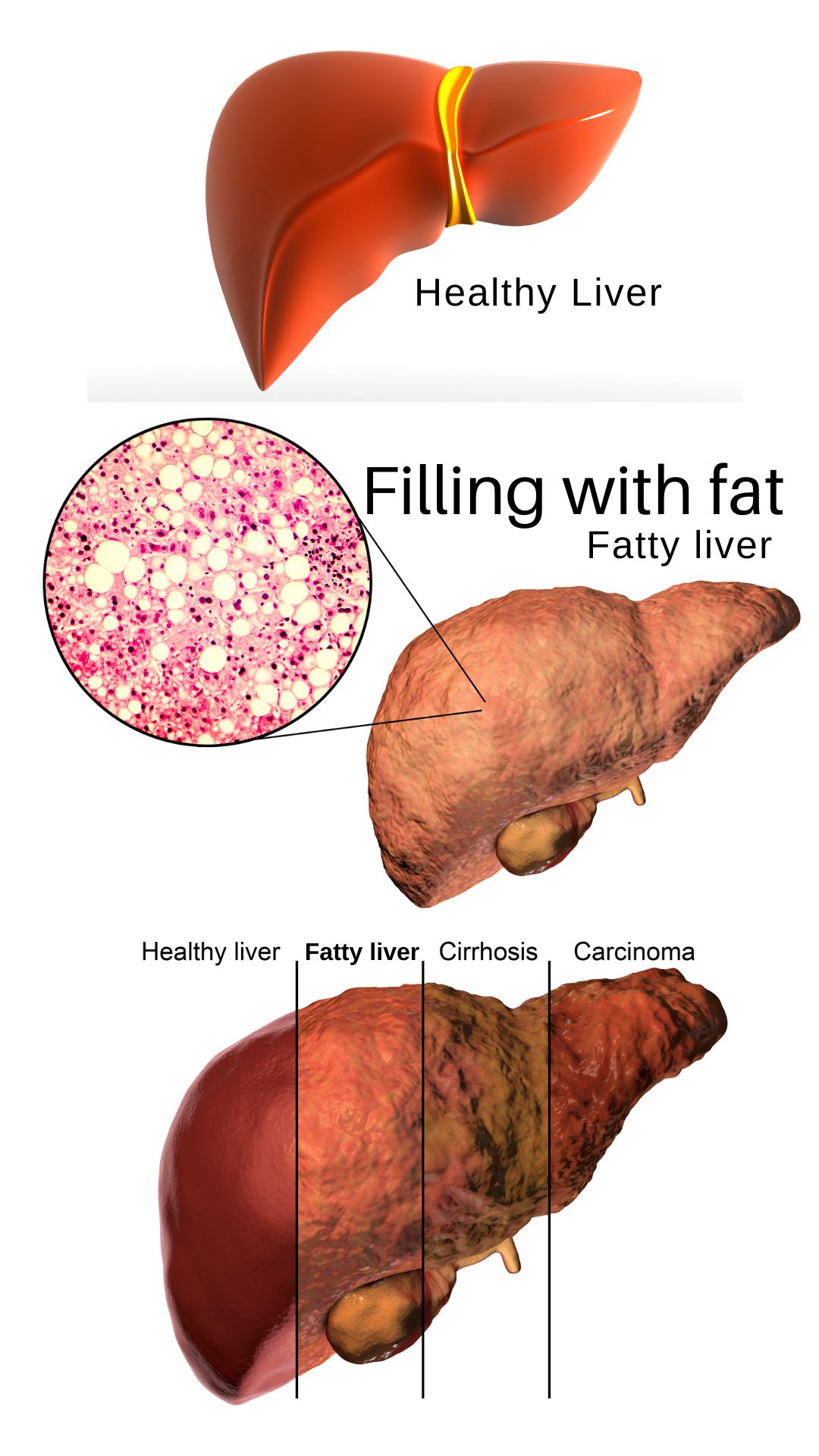
If we do not do anything about our excess sugar and carbs that are filling our liver with fat, then connective tissue of our Liver scars, and Fatty Liver disease develops and then progresses until we make changes.
Here’s the AMAZING news! Fatty liver can be reversed:
Lifestyle and dietary changes are currently the most effective options for managing NAFLD”
(17)
“Lifestyle and dietary changes are currently the most effective options for managing NAFLD” (17)
Learning How to Protect Our Liver Cells
We eat to provide our cells with immediate and longer-term energy. We do need Carbs for our immediate energy needs BUT not in excess.
When we balance the right amount of Carbs for our individual body and activity level, we enjoy a healthy Liver.
Eating for Healthy Liver
Knowing how the body is set up to work (SIMPLIFIED version) empowers us. We can better map out the specifics of what will help us make the Self Care choices that will help us achieve our GOAL. The optimized body that helps us feel good, look good, and LIVE the way we want.
THe simple self care lifestyle
Simplify
How a Fatty Liver Develops
When we eat, our digestive system breaks down the food into molecules. The molecules cross into our bloodstream. When we eat sugar and carbs, they are providing packets of energy that are ready for our cells to use immediately.
A molecule of glucose,….carries a packet of chemical energy just the right size for transport and uptake by cells.
(2)
….it is the ‘deliverable’ form of energy, carried in your blood….to each of your 100 trillion cells.
During this process, molecules of energy (glucose) are released, used, and the excess shuttled into our:
- muscle cells,
- fat cells and
- liver cells.
This is important. First, the sugar molecules are used, and the EXCESS sugar/carbs are shuttled into muscles for immediate and intermediate energy. The EXCESS still not used up is shuttled into Fat cells, and when that has not used up all the EXCESS, the Liver is the target.
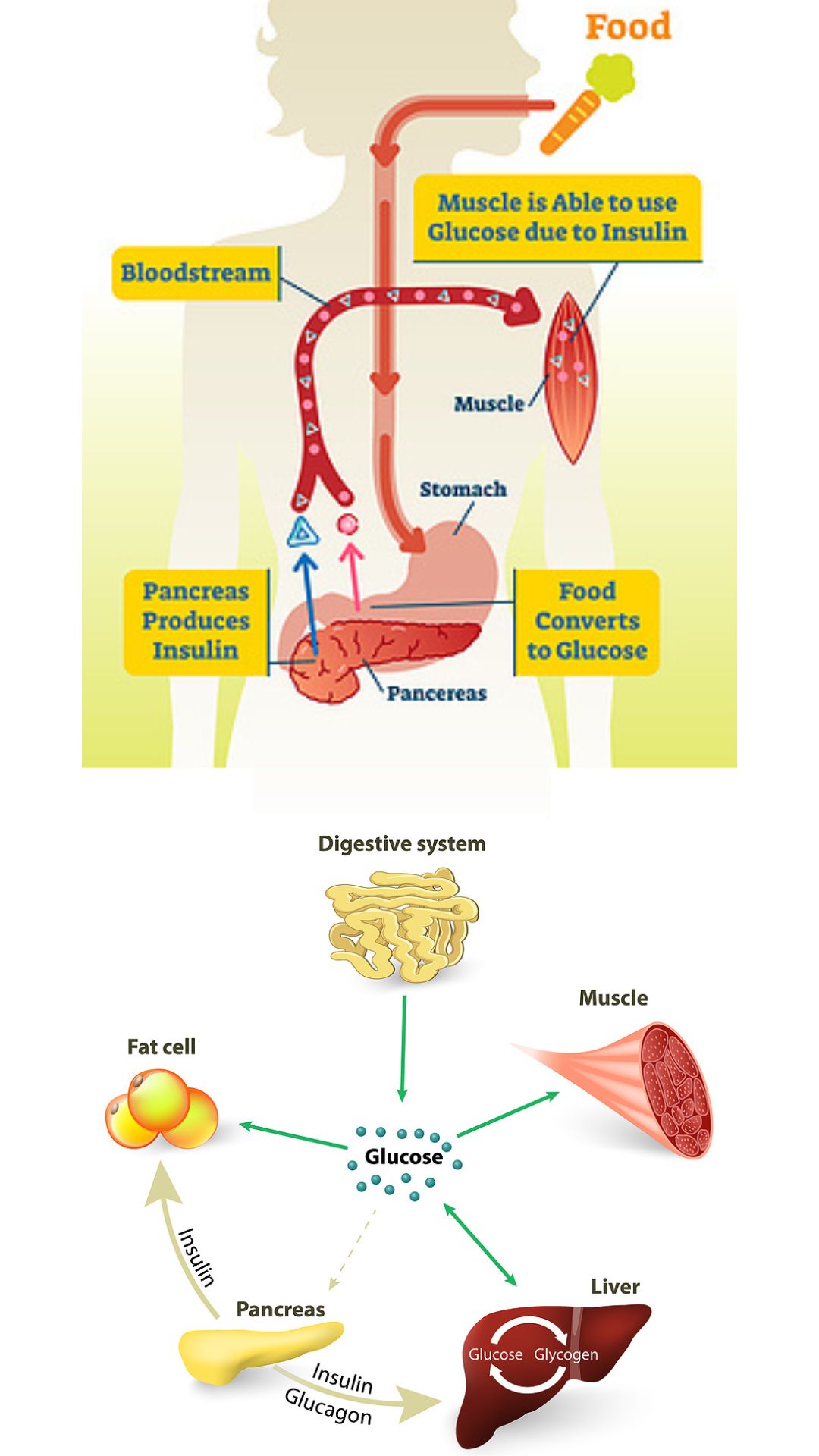
- The ‘energy packet molecule’ (sugar/glucose) provides us with immediate energy.
2. When there is more glucose than the body needs for energy and its storage capacity for molecules of energy (glycogen) has been reached, the liver is prompted to convert the molecule of energy packet (glucose) into triglycerides.
Triglycerides are a type of fat (lipid) found in your blood. When you eat, your body converts any calories it doesn’t need to use right away into triglycerides.
(18)(bold added)
Triglycerides are a type of fat (lipid) found in your blood. When you eat, your body converts any calories it doesn’t need to use right away into triglycerides. (18)(italics and bold added)
BOTTOMLINE: your EXCESS intake of sugars and simple carbohydrates is converted to fat that will be stored and can begin to clog up your Liver.
Under normal circumstances
- Muscles can store a modest amount to use as fuel between meals.
- Our fat cells also get some as a source of energy for our body to pull on when needed.
- And then, the liver stores a small amount. Until there is a constant influx of excess triglycerides. Once the amount of this sugar turned to ‘fat’ (triglyceride) is over what the liver is meant to store, it becomes a stressor on the liver.
Over time, too much excess (triglyceride) fat constantly shuttled into the liver for storage creates the scenario where the liver’s cells gradually get replaced by these fat cells.
This leads to non-alcohol fatty liver disease.
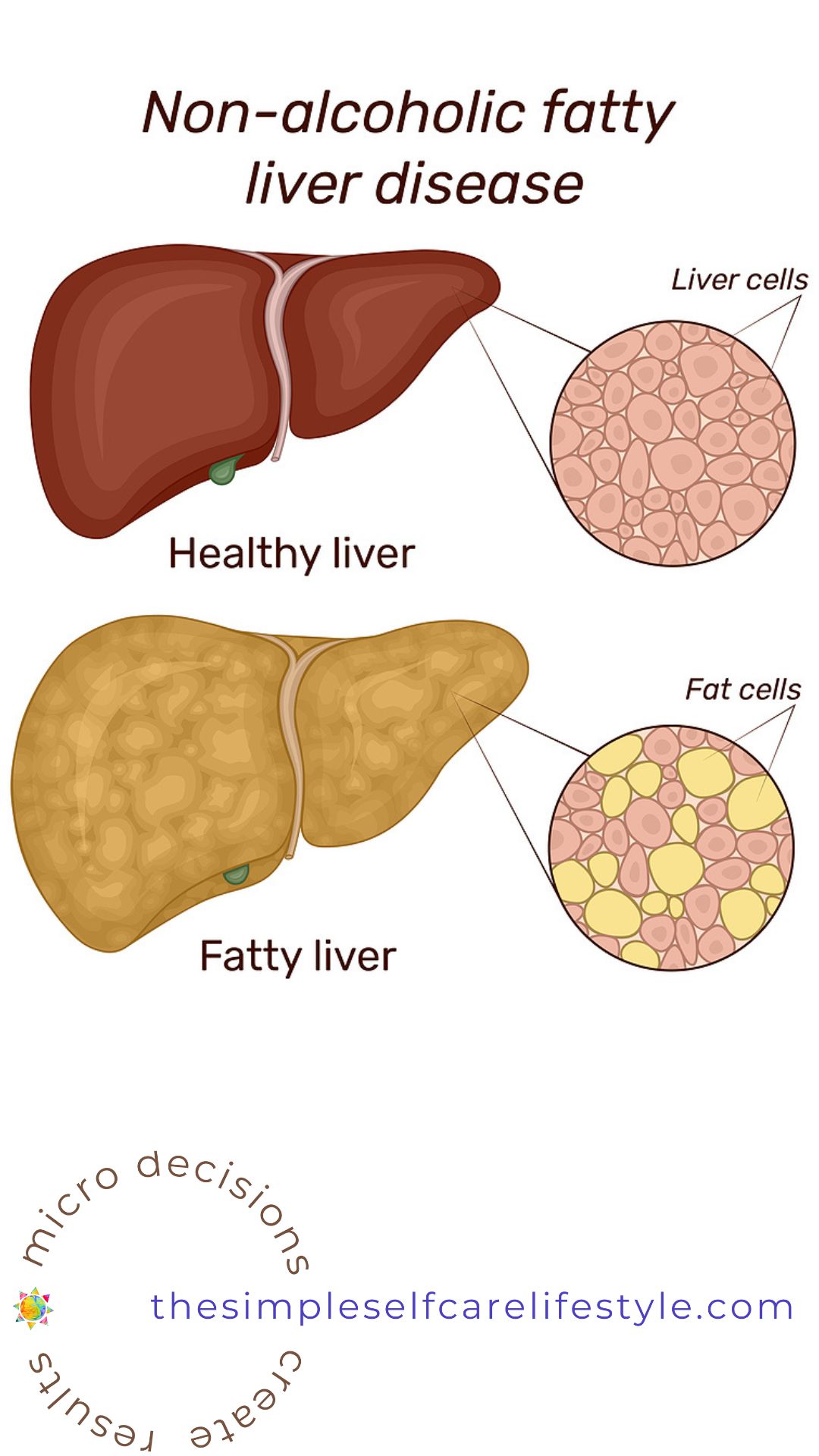
RE-CAP: Fatty Liver Causes
When the liver has too much sugar to process, it converts the extra sugar – or the extra simple carbohydrate to a fat called a triglyceride.
The liver is one of the places that store the excess fat.
Our muscles get some to store, and our fat cells get some to store.
At some point, when the liver is too full of these triglyceride fats to function well, we end up with a fatty liver.
A liver that has too much of this triglyceride fat from eating too much sugar molecules has more and more difficulty doing its many jobs.
The ongoing excess also increases body fat.

Excess Body Fat is also a Contributor to Fatty Liver.
Number 3 on the list of causes of Fatty Liver Disease:
- Sugar
- Simple carbohydrates
- Our body fat, when in excess
Our own excess body fat CAN be a contributor to a fatty liver.
The next step after the fatty liver is established and it is pushed even further without relief from EXCESS sugar, and carbs is the liver replaces its own tissue with connective (scar) tissue, which further reduces its function.
The prevalence rate of NAFLD (Non-alcoholic Fatty Liver Disease) increases with increasing body mass index (BMI).
(3)(4)
“The prevalence rate of NAFLD (Non-alcoholic Fatty Liver Disease) increases with increasing body mass index (BMI).” (3)(4)
“Due to the rising epidemic of obesity in the United States, the prevalence of nonalcoholic fatty liver disease is rapidly increasing and is expected to overtake hepatitis C as the leading indication for liver transplant in the next 30 years” (4)
We Can Avoid This Scenario
Addressing a Fatty Liver as soon as possible can help avoid the progression of liver disease.
Caring for our liver offers many benefits, including reducing our likelihood of experiencing other health problems that liver disease can create.
The liver is a metabolic workhorse that performs a diverse array of biochemical functions necessary for whole-body metabolic homeostasis.
(3)
Why Would A Fatty Liver Lead to Other Health Problems?
Core Concept 1 Our Body is Made Up of Systems. They are Interconnected and DEPENDENT on each other. There is no getting around that.

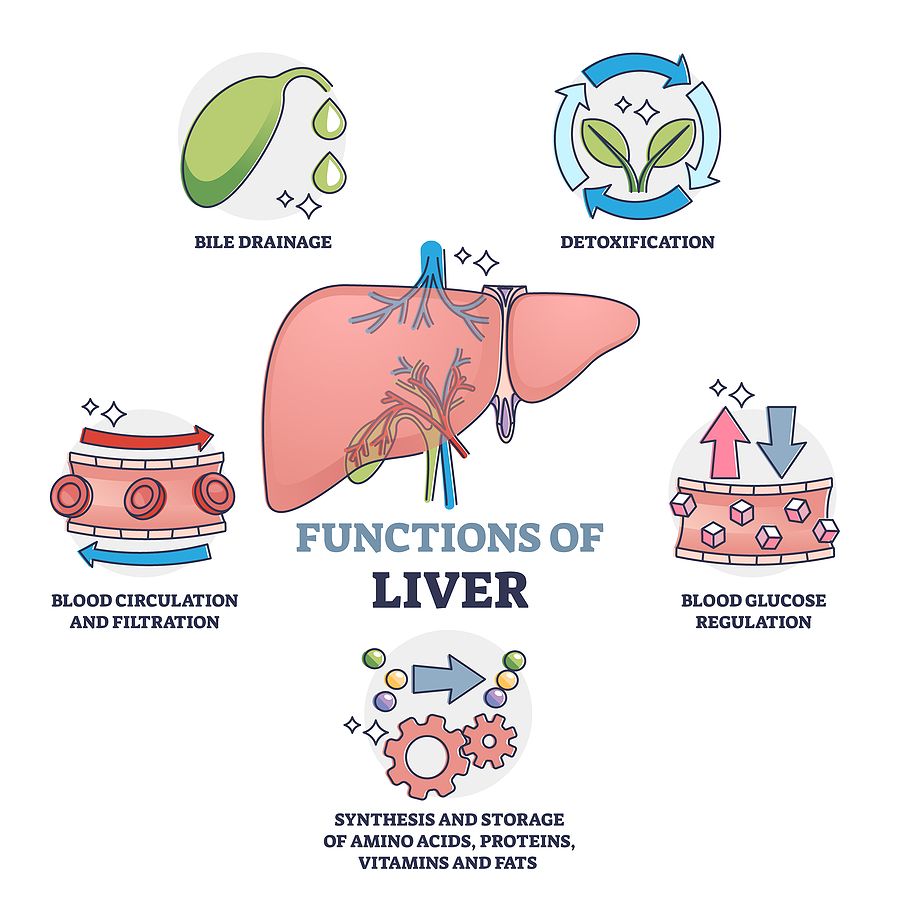
An Organ like our Liver is part of our Digestive system. It removes toxins from our blood, metabolizes nutrients, and impacts our immune system.
You see how having an under-functioning and excessively challenged Liver can impact all our other systems.
Other health problems arise because our liver is needed for pretty much everything that helps to keep our body in balance and working for us.
When our liver is strained, our other systems are strained.
Identifying the causes of a Fatty Liver and reversing the damage improves our lives in exponential ways.
This is why our Simple Self Care Lifestyle hones in on the actions we can take that add up to helping us achieve the 1 GOAL.
Since all our systems are impacted by a Fatty Liver, we FOCUS on and choose Micro Decisions to lighten the stress load on the Liver.
To do that, we need to Leverage the way our body is set up to work so the efforts we put into our Self Care pays off.
When we know how the body is set up, we can cut out confusion about what we should do. This helps us choose the Micro Decisions that’ll have a POSITIVE, supportive impact on our ENTIRE Body. So let’s dive into the SIMPLEST way to begin to address Fatty Liver Causes.
The liver is the largest solid organ in the human body. It is part of the digestive system and plays an essential role in removing toxins from the blood, metabolizing nutrients, and immune function.”
(19)
“The liver is the largest solid organ in the human body. It is part of the digestive system and plays an essential role in removing toxins from the blood, metabolizing nutrients, and immune function.”(19)
Where do we begin?
First, Find The Biggest Culprit of the Fatty Liver Causes: Hidden Sugars.
Relieve the Liver
If possible, we want to relieve the liver from having to handle excess sugar and simple carbs so it does not continue to enlarge with excess triglycerides (a form of fat). (5)(9)
This way, we can avoid disease progression.
Fatty liver should be taken seriously but without panic, because you can slow down and then reverse it.

The Simple Self Care Lifestyle Focus: First Find Hidden Sugar.
The KEY to achieving your goal of caring for your liver is to:
1. Place the focus first on finding and swapping out hidden Sugar.
This first focus may be all it takes.
This is because swapping out hidden sugar can reduce:
- the excess conversion and storage of fatty cells in the liver and
- inflammation and
- excess storage of Body Fat
That is an exponential payoff!
By simplifying our first focus, to the identification and reduction of the most likely of the Fatty Liver Causes, we can simultaneously positively impact 2 other BIG contributors!
Most Common Questions
Q. What About a Special Diet, Supplements, or a Detox?

Special Diet for Fatty Liver:
It is natural for us to immediately look for a way to quickly resolve our fatty liver by following a protocol or ‘liver diet’ found online.
But how long will we stay on it? Will that have us bingeing and stressing our liver even more, when we fall off?
Like quick weight loss plans swinging from ‘being good’ to ‘bingeing’ due to feeling deprived or too restricted is the most likely scenario.
Also, our mood can be negatively influenced if we go on overly restrictive diets. This is often due to sugar addiction withdrawal. (12)
PLUS, Rapid weight loss can make NAFLD worse. (7)
any weight loss should be gradual — no more than a few pounds a week — because losing weight too quickly can actually worsen fatty liver disease.
(7)
We are focused instead on finding YOUR Individual Fatty Liver Causes First Using 4 Steps (There is a pdf below)
Once you find your own personal most probable root causes, you’ll choose which items to slowly swap out. This way
- You can see and pick the one(s) that have the biggest impact.
- And by doing it this way, you will avoid feeling deprived.
- The changes will be lifestyle changes that will allow your liver to heal and stay well life long.

What about Supplements
If I was tested and knew I was low in Vitamin D., I would consider supplementation. This is because normal vitamin D is protective.
“Hypovitaminosis D is associated with the severity and incidence of NAFLD among patients who have normal liver enzymes.”(10)
Hypovitaminosis D is associated with the severity and incidence of NAFLD among patients who have normal liver enzymes.
(10)
As for other supplements, I’d ask my practitioner before adding any.
This is because although research states most vitamins will not do any harm- there is the fact that the liver will need to metabolize the vitamins.
Your practitioner can help you know if you would be adding a burden to your liver.
In general, adding vitamins where there is no known deficiency would be something I’d consider after:
- removing what is stressing my liver and
- with a specific test to pinpoint deficiencies first.
“Even in high doses, most vitamins have few adverse events and do not harm the liver. Many vitamins are normally concentrated in, metabolized by and actually stored in the liver, particularly the fat soluble vitamins. The two exceptions to the lack of harm to the liver by higher doses of vitamins are vitamin A and niacin, both of which can cause distinctive forms of liver injury when taken in high doses.”
(10)

What About A Liver Detox?
Detoxing is defined as:
“a process or period of time in which one rids the body of toxic or unhealthy substances; detoxification”.
This should happen naturally and at a pace that is comfortable to the liver as you find and swap out your excess hidden sugars, excess carbs, and excess consumption.
How Much Sugar Is Excess?
This, of course, varies by:
- how much muscle you have
- your sex
- activity level and
- age
- your ability to metabolize it
In general, the recommendation is
Women: no more than 24 grams Excess Sugar (approx 6 teaspoons) (11)
Men: no more than 36 grams Excess Sugar (approx 9 teaspoons per day) (11)
What does Excess Sugar even mean?
This is sugar outside of the simple carbohydrate food sugar you should eat each day. This is what you find on the labels of every packaged/bagged/processed ‘food’.
The ‘causes of Fatty Liver’ are the most problematic:
- Excess Sugar is the FIRST Focus
- Simple carbohydrates in excess
- Our body fat, when in excess
Figuring out what you should do:
The first step is to focus on Sugar that is not found naturally in foods.
It is the most offensive and most likely culprit when it comes to creating a fatty liver.
And honestly, HIDDEN! How much sugar is in your pizza? Ketchup? Muesli? Diet bar? Corn syrup in your syrup? Coffee creamer? Protein powder?…. Think of anything bought in a box/bag or from a restaurant…You get the picture.
Finding out where your PERSONAL hidden sugar is the key to YOUR success.
How do we figure out how many grams of excess sugar we are eating? We explore our own personal diet.
Here’s How to Know How Much Excess Sugar You Are Consuming.

Step 1.
Write down everything you put in your mouth for the day. And how many times you had it that day.
Do that for a few days – to a week. Here is a sample sheet tracking breakfasts for a week.
Blank pdfs are available for you to download below.

Step 2.
At the end of the week, list the items you ate daily.
Those you consumed 3-6 times during the week.
And those you consumed 1-2 times during the week.

Step 3.
Focus first on what you are consuming daily.
Go through each item on the list and look at the label.
Write down the serving size and the grams of sugar for the serving size.
Continue down the list exploring what has sugar in it.
Here is an example of Step 3.
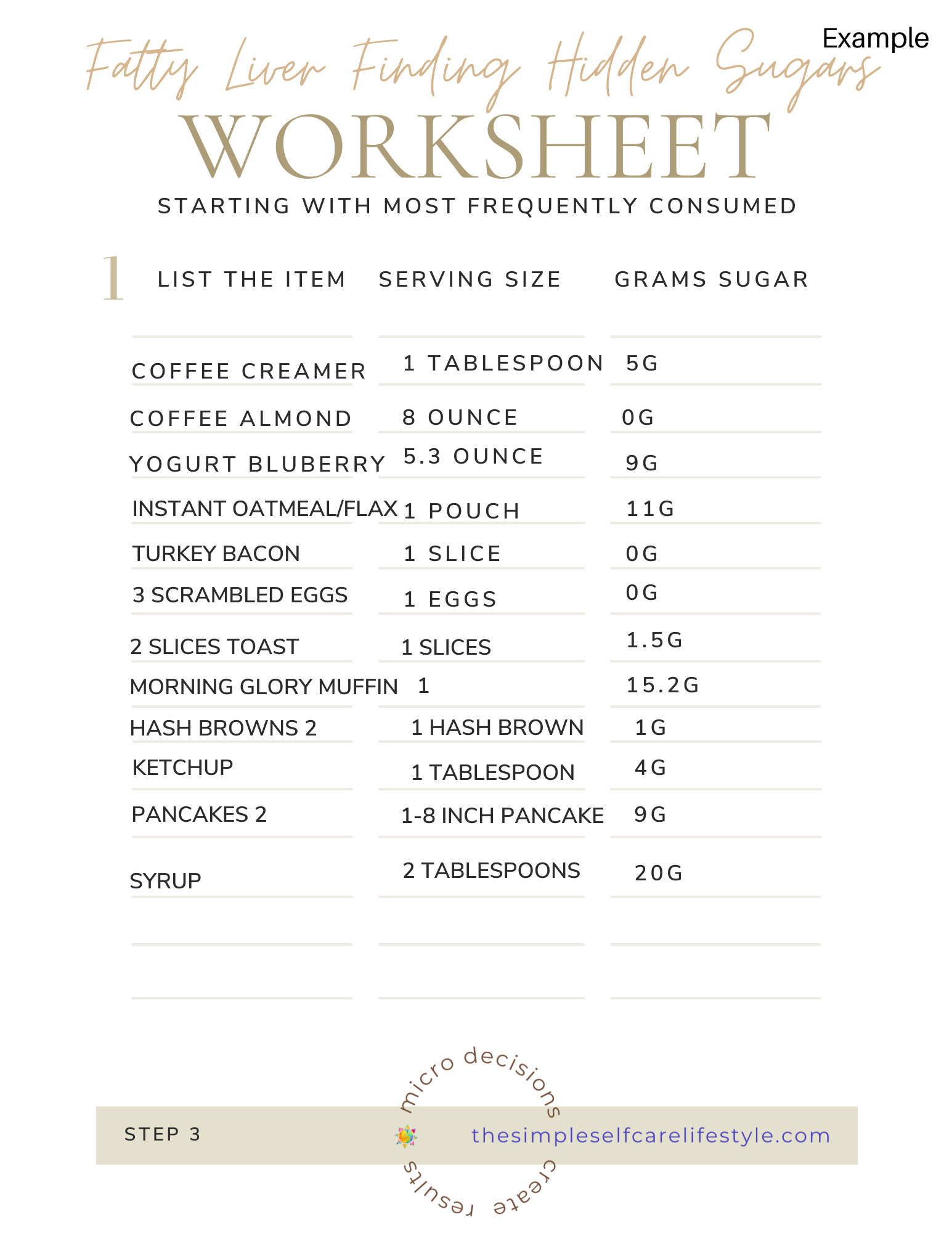
Now I know how much Sugar each of the items I eat has.
Next Step 4.
It is time to figure out if I actually eat the serving size!
This example sheet has actual examples from a client worksheet from many years ago.

By Eliminating 2 Fatty Liver Causes The Fatty Liver Was Able to Heal.
This clients was literally pushing her liver from the time she got up, having almost 4 fold the amount of added sugar already at breakfast! She had NO Idea! NONE!
Hidden sugars started and ended her day.
We saw the morning coffee creamer add to that the daily habit of unwinding from her hectic day with a glass of wine or two and plus a few snacks during the day to take the edge off.
She was able to focus on swapping these 3 things instead of following ‘someone else’s detox diet’. She found the process eye-opening, SIMPLE- NOT always easy but SIMPLE and straightforward to do.
Finding the hidden sugar changed everything about how she went about reducing her fatty liver and excess weight she had been trying for DECADES it was now reducing.
The reduction in hidden sugar helped her metabolism, which helped her Liver even more. This is because supporting her liver was simultaneously helping her to Optimize Her Body. The KEY to ALL our Goals!
Understanding What Was Impacting Her Specific Body Made All The Difference.
Understanding what was going on and that she had control helped her overcome her frustration and anxiety about what to eat.
Also, reducing the fear that something was very wrong with her body was helpful to her.
This, of course, helped her HPA axis, which helped her OVER all wellness!
Not only that but the How Your Body Uses Body Fat Part 1 and Part 2 made COMPLETE sense to her after using the Finding Hidden Sugars Worksheets!
And the post on One of the Worlds Healthiest Foods: Flaxseed helped as well because:
Our data indicate that FLAX can be a promising functional food for preventing NASH through regulating microbiomes and BAs.
“Our data indicate that FLAX might be a promising functional food for preventing NASH through regulating microbiomes and BAs.”
NASH, is the most severe form of nonalcoholic fatty liver disease (NAFLD). Flax happens to be listed as one of the world’s healthiest foods. It is easy to use, and research states it has a multitude of benefits.
Success! Fatty Liver Resolved.
A few SIMPLE changes, and she got her Liver & Body back on track.
Knowing how to calculate the hidden sugars can make a world of difference.
It SIMPLIFIES your plan of action and makes the path for you much clearer. Try using the worksheets to find your hidden sugars. It is a great first step!
Worksheets to Help Make the First Steps Simpler.
Downloadable: The Worksheet Packet to help you to uncover your Liver stressors.


email: [email protected]
Two Other Posts that may interest you and more below the References and Resources Section.
The Simple Self Care Lifestyle
THe simple self care lifestyle
Simplify
self care
Post categories





SHOP Products
Personal Products
Healthy Home
Quality Supplements
Things to Keep Handy
Quality Food Sources
Simple Self Care Programs
I’M GLAD YOU ARE HERE!

Additional Posts about Your Body Below these Linked References/Resources for you